Getting vaccines to everyone, everywhere
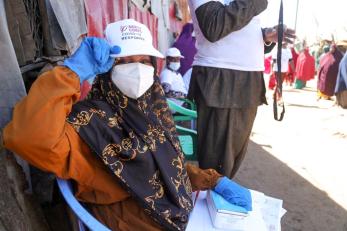
The COVID‑19 pandemic has been called the greatest public health challenge of our generation. For months, while millions of people have suffered and died from this deadly disease, the world has awaited a reprieve in the form of effective vaccines. Now that they’re finally starting to roll out, there are many glaring questions and challenges, particularly around equity in distribution.
In dozens of lower-income countries, only one in 10 people can hope to receive a vaccine by the end of this year, not even close to the number needed to comprehensively vaccinate at-risk groups. In contrast, wealthy nations have bought enough COVID‑19 vaccine doses to vaccinate their entire populations three times over by the end of 2021. And people in refugee communities are likely to be among the last to receive the vaccines.
We believe that vaccines should be available to everyone, everywhere.
Getting everyone vaccinated will require a collaborative effort to build trust in the vaccine and those who provide it, particularly in conflict zones and among vulnerable populations. Read on for more about how we plan to tackle these challenges—and what you can do to help:
- Are the COVID‑19 vaccines reaching the world’s most vulnerable communities?
- What is preventing the vaccines from reaching the world’s most vulnerable people?
- What is being done to ensure equitable global vaccine distribution?
- Why don’t some communities trust the vaccines?
- What kind of misinformation is being spread about COVID‑19 and the vaccines?
- What will it take to overcome distrust of the vaccines?
- How is Mercy Corps combating misinformation and helping to build trust in the vaccines?
- What can be done, by Mercy Corps and others, to make the vaccines more widely available to the most vulnerable communities?
- What can I do to help?
Are the COVID‑19 vaccines reaching the world’s most vulnerable communities?
Wealthy nations representing just 14% of the world’s population own over half of the most promising vaccines. This means the most vulnerable people in the world — including refugees, marginalized groups and people living in conflict zones — risk being left behind unless urgent action is taken to make sure enough doses are manufactured.
In addition, vast parts of the world lack the refrigeration and infrastructure to administer an effective vaccination program, creating additional hurdles to reaching vulnerable communities.
Fortunately, efforts are underway to address these inequities. International organizations are overseeing the installation of a vast number of solar-powered vaccine refrigerators in order to uphold what’s referred to as the cold chain — a supply chain of temperature-sensitive products — in developing countries. UNICEF plans to get 520 million syringes to the developing world ahead of COVID‑19 vaccines to help with initial supply. And Pfizer plans to release its vaccine in a powdered form, which will require standard refrigeration as opposed to special freezers, enabling more vaccines to get into the hands of people in developing nations.
What is preventing the vaccines from reaching the world’s most vulnerable people?
In addition to the unequal vaccine distribution and lack of reliable electricity, there’s also a potential for supply chains to break down the farther vaccines travel, and a lack of dependable transportation in some places can make it harder for people to reach clinics and actually receive the vaccinations. Conflict zones make it even more difficult for health care professionals and aid workers to safely reach civilians and deliver vaccines.
One of the biggest obstacles, though, is less tangible: convincing people that vaccines — and those providing them — can be trusted.
Studies indicate that large swaths of people are hesitant to get the vaccine in the first place. Even before COVID‑19 was discovered, vaccine hesitancy was named one of the top 10 global health threats in 2019 by the World Health Organization.
This is especially true in conflict zones where governance is weak and trust in institutions is low.
Persuading people to trust the vaccine will require humanitarian groups, governments and public health experts to work together to dispel myths and provide reliable information.

What is being done to ensure equitable global vaccine distribution?
One of the biggest efforts underway is a global initiative called COVAX, which aims to provide countries worldwide access to safe, effective vaccines — currently, 189 countries have joined.
COVAX’s success will ultimately be dependent on funding from rich countries, and is still lacking the funds it needs to fully succeed. Despite that, COVAX has already secured 700 million vaccine doses to be distributed around the world, and plans to make at least 2 billion more vaccine doses available by next year.
In addition, we are calling on drug companies working on COVID‑19 vaccines to share their technology so additional doses can be produced and made available to those in need.
Why don’t some communities trust the vaccines?
Misinformation about vaccines is rampant. It spreads through word of mouth, traditional media and social media—a particularly rich breeding ground for false information.
In conflict zones, public distrust is especially rampant because people have often experienced neglect, chronic poverty, discrimination and corruption, sometimes at the hands of their own governments. When people understand public health systems to be a function of these governments, this lack of trust can quickly thwart vaccination campaigns.
In addition, the hurried timeline for these vaccines is a factor. While the COVID‑19 vaccines have been tested for effectiveness and safety, it’s natural for some to be skeptical of the unknown.
What kind of misinformation is being spread about COVID‑19 and the vaccines?
Unfortunately, the array of misinformation out there is extensive. In Kenya, short videos and memes have emerged online and in closed messaging groups claiming that COVID‑19 doesn’t exist at all, and that the government is fabricating the number of cases in order to get funding from international donors. In Libya, some people believe the pandemic is a ploy to allow authorities to embezzle public funds. In Puerto Rico, rumors are circulating that people should abstain from consuming alcohol within 40 days of taking the vaccine.
Other conspiracy theories floating around about COVID‑19 vaccines include that the injections may contain surveillance microchips; that vaccines will be a larger risk than getting the disease itself; and that it will alter people’s DNA.
This type of misinformation is widespread around the world, in rich countries and poor countries alike.

What will it take to overcome distrust of the vaccines?
Massive and well-managed community engagement and trust-building campaigns are imperative. They must be centered on understanding people’s prior experiences with their public health systems and governments, and then providing them with factual information.
Reaching people through local avenues is much more effective than simply disseminating information using top-down approaches. All too often, campaigns to educate people about vaccines or broader public health interventions do not engage communities in meaningful ways.
We need to get youth and women’s groups, businesses, local civil society, and traditional and religious leaders on board to help design and implement grassroots initiatives that will build trust in vaccinations and strengthen relationships between communities and their governments. We need to meet people where they are, which means taking all of their previous experiences and biases into account and reaching them through personal interactions.
As Mercy Corps CEO Tjada D'Oyen McKenna has written, through these coordinated efforts, “We can help restore trust in a way that supports both effective vaccine delivery and lasting peace.”

How is Mercy Corps combating misinformation and helping to build trust in the vaccines?
In many of our programs, we’ve already been working to combat misinformation around COVID‑19. This entails understanding what kind of information is out there and how people are getting it, and then countering that with accurate information through trusted channels.
In northeast Nigeria, we are addressing misinformation about COVID‑19 by piloting a “Rumor Tracker” tool that allows citizens to report rumors they hear in their communities via text message and phone calls, so that we can get a sense of what specific misinformation is out there. We’ve also recruited “truth champions”-- local leaders who are trained on how to respond to rumors with accurate information.
Last year, in Haiti, we implemented a text and voicemail campaign sharing messages and dispelling rumors about the virus — it reached 2.2 million Haitians. We plan to reboot the platform with new content specifically about the vaccine.
Similarly, in Colombia, we’re adapting a social media campaign we created to provide accurate information about COVID‑19 to now include accurate information about the vaccine.
In order to combat fear around isolation and care centers in Zimbabwe, we produced survivor stories to dispel misinformation about how COVID‑19 is spread, what the symptoms are, and how treatment works.
We have other efforts underway in Puerto Rico, Iraq and the DRC, where we are empowering community leaders to get accurate information out there through grassroots campaigns.
What can be done, by Mercy Corps and others, to make the vaccines more widely available to the most vulnerable communities?
We believe organizations like Mercy Corps have a critical role to play in ensuring vaccines reach vulnerable people in the 40+ countries where we work. It’s important for the communities we serve to know that we are here to help.
The World Health Organization and governments should partner with and fund organizations already on the ground — especially those with an established and trusted local presence preceding the pandemic — to create and instill campaigns that will build trust in vaccines.

What can I do to help?
The best way to help is to give. Contribute today to help Mercy Corps protect the world’s most vulnerable people against COVID‑19, meet immediate needs, and prepare for the devastating impact of economic shock that will push people further into crisis.


